  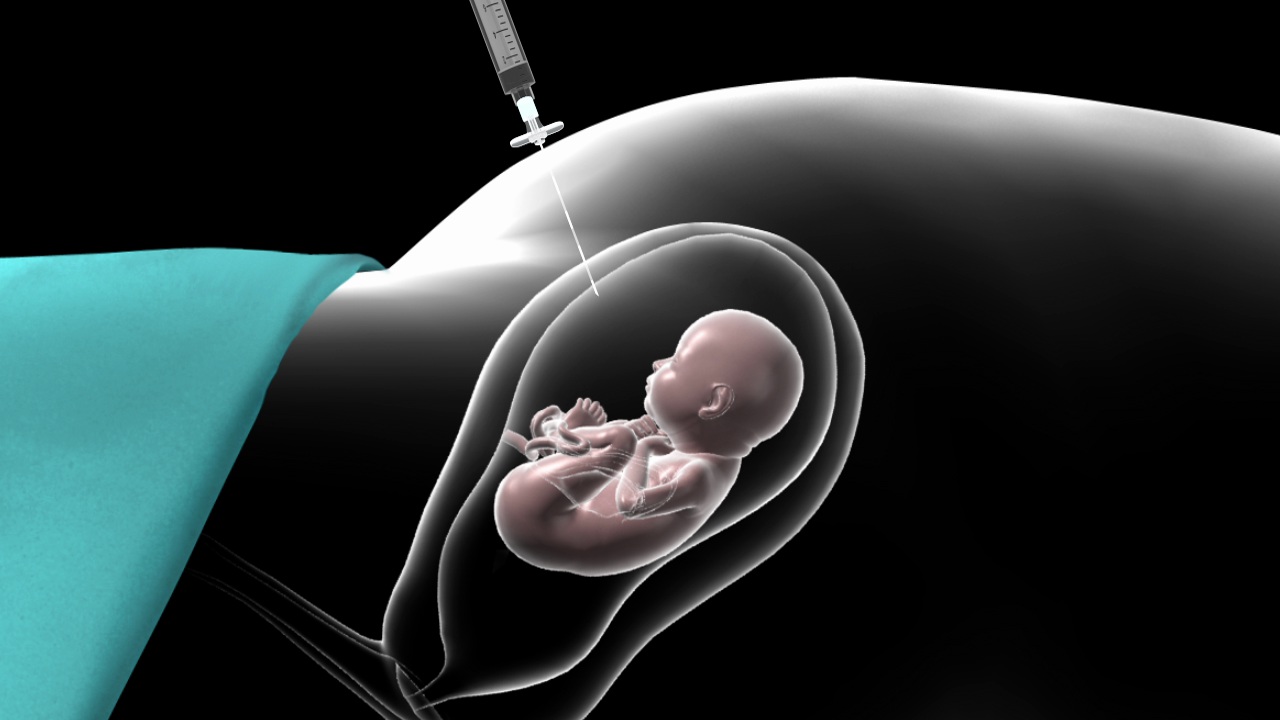 
What Happens to the Twin Babies Affected by TTTS? Studies show a higher rate of identical twins (up to 20 times with IVF) in women having these treatments than occur naturally. Since spontaneous pregnancy loss (spontaneous abortion) and pregnancy terminations (elective abortions) that occur prior to 20 weeks go uncounted by the C.D.C., our estimate of TTTS cases may be very conservative.Īlthough infertility treatments have increased the rate of multiple birth, they have not diluted the expected incidence of identical twins even though multiple embryos are often produced and implanted. 15 = 4,568 cases of TTTS per year in U.S. The majority of identical twins share a common (monochorionic) placenta, and of these approximately 15% go on to develop TTTS.īy extrapolating the number of expected identical twins (about one-third) from annual multiple births, and the number of twins with monochorionic placentas (about two-thirds), and from these the number thought to develop TTTS (about 15%), there are at least 4,500 TTTS cases per year in the U.S. Acute TTTS twins may have a better chance to survive based on their gestational age, but may have a greater chance of surviving with handicaps.īased on 2005, similar to 2018, USA National Center for Health Statistics (4,138,349 total births), the rate of multiple births per year is now 1:30 (3.4%), or approximately 139,816 twins or higher multiples. This may occur in labor at term, or during the last third of pregnancy whenever one twin becomes gravely ill or even passes away as a result of the abnormalities in their shared placenta. Acute TTTS describes those cases that occur suddenly, whenever there is a major difference in the blood pressures between the twins. Without treatment, most of these babies would not survive and of the survivors, most would have handicaps or birth defects. In addition, the twins will have a longer time during their development in the womb to be affected by the TTTS abnormalities. These cases are the most serious because the babies are immature and cannot be delivered. Chronic TTTS describes those cases that appear early in pregnancy (12-26 weeks’ gestation). The placental abnormalities determine when and to what degree a transfusion occurs between the twins. TTTS can occur at any time during pregnancy, even while a mother is in labor at term. This excess blood puts a strain on this baby’s heart to the point that it may develop heart failure, and also causes this baby to have too much amniotic fluid (polyhydramnios) from a greater than normal production of urine. The recipient twin becomes overloaded with blood. This in turn leads to slower than normal growth than its co-twin, and poor urinary output causing little to no amniotic fluid or oligohydramnios (the source of most of the amniotic fluid is urine from the baby). The transfusion causes the donor twin to have decreased blood volume. Depending on the number, type and direction of the connecting vessels, blood can be transfused disproportionately from one twin (the donor) to the other twin (the recipient). 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
